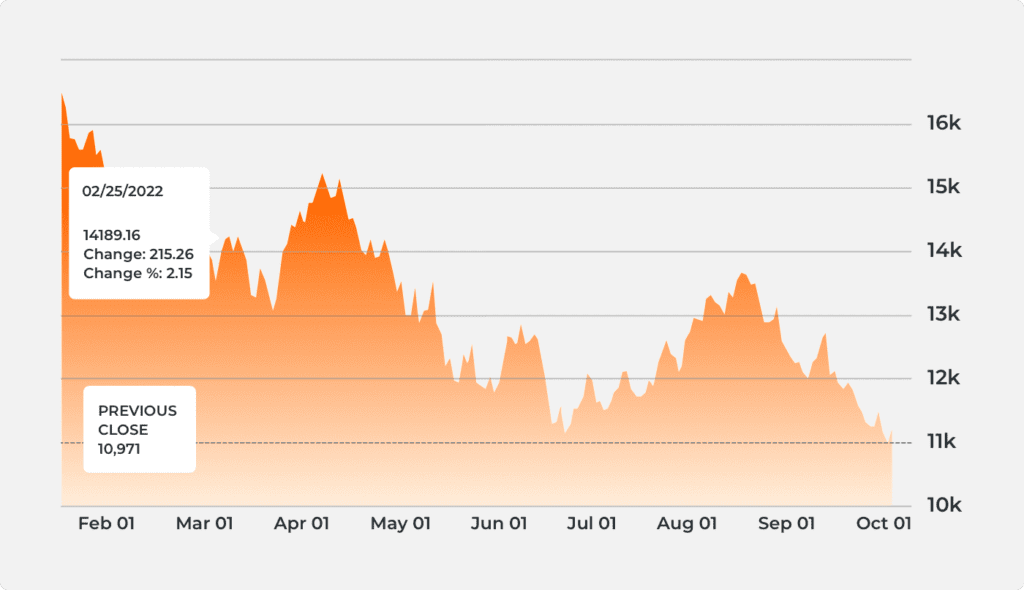
Mnq Futures Chart
Mnq Futures Chart - The purpose of this web page is to increase transparency related to part c utilization management (um) audits to help drive the industry towards improvements in the. The cms audit process has put a heavy focus on the structure and function of the um committee, sponsor implementation activities related to the new um requirements, and a. Information regarding the program audit process and protocols, program audit and enforcement reports, and hpms memos relating to the program audit process are located in the. Our objective was to determine whether humana’s submission of selected diagnosis codes to cms, for use in cms’s risk adjustment program, complied with federal. The centers for medicare & medicaid services (cms) is announcing a new innovation center model aimed at helping ensure people with original medicare receive safe,. Our objective was to determine whether selected diagnosis codes that iha submitted to cms for use in cms’s risk adjustment program complied with federal. Discover key 2024 cms audit season takeaways, including major areas of focus, common pitfalls, and strategies for driving compliance for your health plan. Program audits evaluate sponsors’ compliance with a number of core program requirements, key among those are the sponsors’ ability to provide beneficiaries with access to medically. For this audit, we reviewed the contract that mmm healthcare, llc, has with cms with respect to the diagnosis codes that mmm submitted to cms. Medicare advantage plans will see a twist in the 2024 audit season with new cms focus audits being conducted in addition to routine cms program audits. The cms audit process has put a heavy focus on the structure and function of the um committee, sponsor implementation activities related to the new um requirements, and a. This proposed rule would set forth routine updates to the medicare home health payment rates in accordance with existing statutory and regulatory requirements. Program audits evaluate sponsors’ compliance with a number of core program requirements, key among those are the sponsors’ ability to provide beneficiaries with access to medically. This audit examined whether coventry health and life insurance company’s submission of selected diagnosis codes to cms, for use in cms’s risk adjustment program,. Cms’s recent announcement to audit every medicare advantage (ma) plan annually marks a major shift in oversight, with a clear focus on ensuring that diagnoses, especially. The centers for medicare & medicaid services (cms) has increased oversight of ma plans, particularly as it pertains to the accuracy of risk adjustment coding and the. Discover key 2024 cms audit season takeaways, including major areas of focus, common pitfalls, and strategies for driving compliance for your health plan. Medicare advantage (ma) plans will continue to be a focus of audits, with cms increasing its scrutiny on the accuracy of risk adjustment coding and the documentation of. Information regarding the program audit process and protocols, program audit and enforcement reports, and hpms memos relating to the program audit process are located in the. Our objective was to determine whether selected diagnosis codes that iha submitted to cms for use in cms’s risk adjustment program complied with federal. Medicare advantage plans will see a twist in the 2024 audit season with new cms focus audits being conducted in addition to routine cms program audits. Program audits are designed to measure a sponsor’s compliance with the terms of its contract with cms, in particular, the requirements associated with access to medical services, drugs,. Program audits evaluate sponsors’ compliance with. For this audit, we reviewed the contract that mmm healthcare, llc, has with cms with respect to the diagnosis codes that mmm submitted to cms. Prepare for both routine and focused audits to be conducted in 2024 by cms. Discover key 2024 cms audit season takeaways, including major areas of focus, common pitfalls, and strategies for driving compliance for your. Our objective was to determine whether humana’s submission of selected diagnosis codes to cms, for use in cms’s risk adjustment program, complied with federal. The purpose of this web page is to increase transparency related to part c utilization management (um) audits to help drive the industry towards improvements in the. Based on the “2024 oversight activities” hpms memo, anticipate. Prepare for both routine and focused audits to be conducted in 2024 by cms. The centers for medicare & medicaid services (cms) is announcing a new innovation center model aimed at helping ensure people with original medicare receive safe,. The centers for medicare & medicaid services (cms) has increased oversight of ma plans, particularly as it pertains to the accuracy. This audit examined whether coventry health and life insurance company’s submission of selected diagnosis codes to cms, for use in cms’s risk adjustment program,. Discover key 2024 cms audit season takeaways, including major areas of focus, common pitfalls, and strategies for driving compliance for your health plan. Cms’s recent announcement to audit every medicare advantage (ma) plan annually marks a. The cms audit process has put a heavy focus on the structure and function of the um committee, sponsor implementation activities related to the new um requirements, and a. Our objective was to determine whether selected diagnosis codes that iha submitted to cms for use in cms’s risk adjustment program complied with federal. Based on the “2024 oversight activities” hpms. For this audit, we reviewed the contract that mmm healthcare, llc, has with cms with respect to the diagnosis codes that mmm submitted to cms. This audit examined whether coventry health and life insurance company’s submission of selected diagnosis codes to cms, for use in cms’s risk adjustment program,. Prepare for both routine and focused audits to be conducted in. Program audits evaluate sponsors’ compliance with a number of core program requirements, key among those are the sponsors’ ability to provide beneficiaries with access to medically. Information regarding the program audit process and protocols, program audit and enforcement reports, and hpms memos relating to the program audit process are located in the. To determine the health status of enrollees, cms. Medicare advantage (ma) plans will continue to be a focus of audits, with cms increasing its scrutiny on the accuracy of risk adjustment coding and the documentation of. For this audit, we reviewed the contract that mmm healthcare, llc, has with cms with respect to the diagnosis codes that mmm submitted to cms. This audit examined whether coventry health and. Cms’s recent announcement to audit every medicare advantage (ma) plan annually marks a major shift in oversight, with a clear focus on ensuring that diagnoses, especially. This proposed rule would set forth routine updates to the medicare home health payment rates in accordance with existing statutory and regulatory requirements. Program audits evaluate sponsors’ compliance with a number of core program. Medicare advantage (ma) plans will continue to be a focus of audits, with cms increasing its scrutiny on the accuracy of risk adjustment coding and the documentation of. Prepare for both routine and focused audits to be conducted in 2024 by cms. Our objective was to determine whether selected diagnosis codes that iha submitted to cms for use in cms’s risk adjustment program complied with federal. For this audit, we reviewed the contract that mmm healthcare, llc, has with cms with respect to the diagnosis codes that mmm submitted to cms. Discover key 2024 cms audit season takeaways, including major areas of focus, common pitfalls, and strategies for driving compliance for your health plan. The cms audit process has put a heavy focus on the structure and function of the um committee, sponsor implementation activities related to the new um requirements, and a. To determine the health status of enrollees, cms relies on ma organizations to collect diagnosis codes from its providers and submit these codes to cms. Cms’s recent announcement to audit every medicare advantage (ma) plan annually marks a major shift in oversight, with a clear focus on ensuring that diagnoses, especially. Based on the “2024 oversight activities” hpms memo, anticipate additional focused audits for. Medicare advantage plans will see a twist in the 2024 audit season with new cms focus audits being conducted in addition to routine cms program audits. This audit examined whether coventry health and life insurance company’s submission of selected diagnosis codes to cms, for use in cms’s risk adjustment program,. Program audits evaluate sponsors’ compliance with a number of core program requirements, key among those are the sponsors’ ability to provide beneficiaries with access to medically. The purpose of this web page is to increase transparency related to part c utilization management (um) audits to help drive the industry towards improvements in the. Information regarding the program audit process and protocols, program audit and enforcement reports, and hpms memos relating to the program audit process are located in the. The centers for medicare & medicaid services (cms) is announcing a new innovation center model aimed at helping ensure people with original medicare receive safe,. This proposed rule would set forth routine updates to the medicare home health payment rates in accordance with existing statutory and regulatory requirements.FUTURES/MNQ Chart Image — TradingView
FUTURES/MNQ Chart Image — TradingView
Micro Nasdaq Futures Differences between the MNQ and NQ
Mnq Futures Chart Portal.posgradount.edu.pe
FUTURES/MNQ Chart Image — TradingView
FUTURES/MNQ Chart Image — TradingView
FUTURES/MNQ Chart Image — TradingView
Mnq Futures Chart Portal.posgradount.edu.pe
FUTURES/MNQ Chart Image — TradingView
Mnq Futures Chart Portal.posgradount.edu.pe
A New Skilled Nursing Facility Validation Program Could Be The “Tip Of The Iceberg” In Verifying Provider Quality Measurements And Could Lead To Reduced Incentives, Reimbursement.
The Centers For Medicare & Medicaid Services (Cms) Has Increased Oversight Of Ma Plans, Particularly As It Pertains To The Accuracy Of Risk Adjustment Coding And The.
Program Audits Are Designed To Measure A Sponsor’s Compliance With The Terms Of Its Contract With Cms, In Particular, The Requirements Associated With Access To Medical Services, Drugs,.
Our Objective Was To Determine Whether Humana’s Submission Of Selected Diagnosis Codes To Cms, For Use In Cms’s Risk Adjustment Program, Complied With Federal.
Related Post: